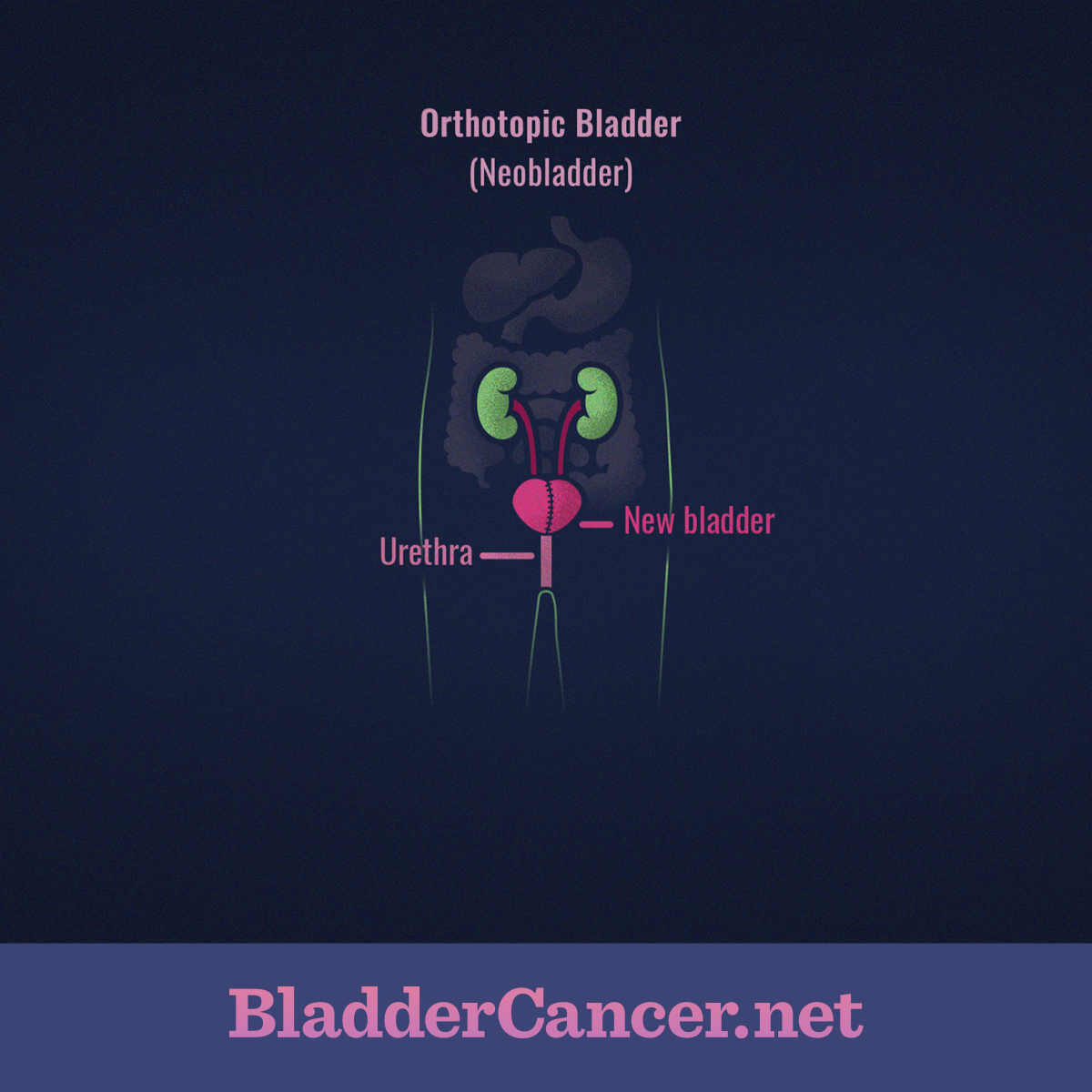
Living With a Neobladder
Reviewed by: HU Medical Review Board | Last review date: September 2017. | Last updated: December 2024
Patients who have invasive bladder cancer may need to have a type of surgery called radical cystectomy.1 Invasive bladder cancer is diagnosed if the cancer cells have grown into the muscle in the wall of the bladder, or if there are tumors located in more than one area of the bladder. During a radical cystectomy, the surgeon typically removes the patient’s entire bladder, part of the ureters (the thin tubes that connect the bladder to the kidneys), and the lymph nodes that surround the bladder. In male patients, the surgeon usually removes the prostate and seminal vesicles in addition to the bladder, parts of the ureters, and lymph nodes. In female patients, the surgeon may also remove the uterus, ovaries, fallopian tubes, cervix, and sometimes part of the vagina.
What is a neobladder?
After the patient’s bladder is removed, the surgeon typically uses reconstructive surgery to create a different way for urine to be stored and passed from the patient’s body. There are several different ways to create another route for urine to be stored and passed from the body, one of which is called a neobladder. Your healthcare providers will talk with you about whether a neobladder is a good option for you. It is usually recommended only for patients who have a low risk that cancer will grow again in the urethra after treatment is completed.
How is it made?
The surgeon creates a neobladder out of a small part of the patient’s own intestine. The neobladder is a reservoir or pouch that is connected one end to the patient’s ureters, which are thin tubes that carry urine out of the kidneys. In this way, the urine drains through the ureters and into the neobladder. The other end of the neobladder is connected to the patient’s urethra. The urethra is the thin tube that connects to the bladder and allows stored urine to pass out of the body.
How does it work?
Compared to other options for reconstructive surgery, the neobladder works in a way that is most similar to the function of the normal bladder.1 In patients with a neobladder, urine passes from the kidneys to the ureters and into the neobladder pouch. To empty the neobladder, the patient contracts his or her abdominal muscle to push the urine in the neobladder out of the body through the urethra. Most male patients find that it is easier to do this while sitting down.
What are the advantages?
There are advantages and disadvantages to each of the different options available after a radical cystectomy.1 For many patients, the main benefit of the neobladder is that emptying urine from the neobladder is most similar to the normal process of urination than the other options of incontinent diversion (ileal conduit) and continent diversion (Indiana pouch reservoir).
What are the disadvantages?
However, the neobladder option does have some disadvantages to be considered. The surgery it requires is longer and more complex than the surgery required for an ileal conduit. After surgery, most patients will experience urine leakage (incontinence) that can last for up to six months. Urine leakage can occur during the day and/or night, and some patients may need to wear a pad to absorb the urine.
Some patients may also have difficulty fully emptying the neobladder using their abdominal muscles. These patients may need to use a catheter several times a day to empty the bladder, especially in the months after surgery, but potentially for a longer period of time. A catheter is a thin, flexible tube that is inserted into the neobladder through the urethra to empty the urine stored there. This is necessary because urine that is stored in the bladder for too long can grow bacteria that can cause infections.
Adjusting to life with a neobladder
After recovering from surgery, it takes some time for most patients to adjust to living with a neobladder.2,3 One challenge is learning when and how to use your abdominal muscles to empty the neobladder. Normally the bladder is connected to nerves that signal to a person that the bladder needs to be emptied. However, the neobladder does not have the same nerve connections. It generally takes time to understand the new signals that indicate when you need to urinate. Your healthcare providers will help you understand your body’s new signals. Urine that is stored in the neobladder may also contain white mucus because the neobladder is made out of intestinal tissue.
Over time, most patients find that they are able to resume most, if not all, of their day-to-day activities, including physical exercise and sexual activities. Unless their work involves certain types of strenuous activities, most people will be able to go back to work as usual.
What are the side effects?
A common side effect of the neobladder is urine leakage. Some people find that it is more common during certain types of activities, such as lifting something heavy. Some ways to help address this issue are to empty your bladder more often and use pelvic floor exercises to help strengthen the muscles around the urethra, which can reduce leaking. Your healthcare providers can provide other advice about ways to deal with and reduce leaking.